Getting Started with Your Team
Adding team members allows you to distribute workload, manage individual staff schedules, and assign specific services to the right providers. This is essential for scaling your practice and ensuring clients are always booked with the most appropriate clinician.
Creating a New Team Member
- Click Settings on the navigation pane.
- Select Team.
- Click Add Team Member at the top right of the screen.
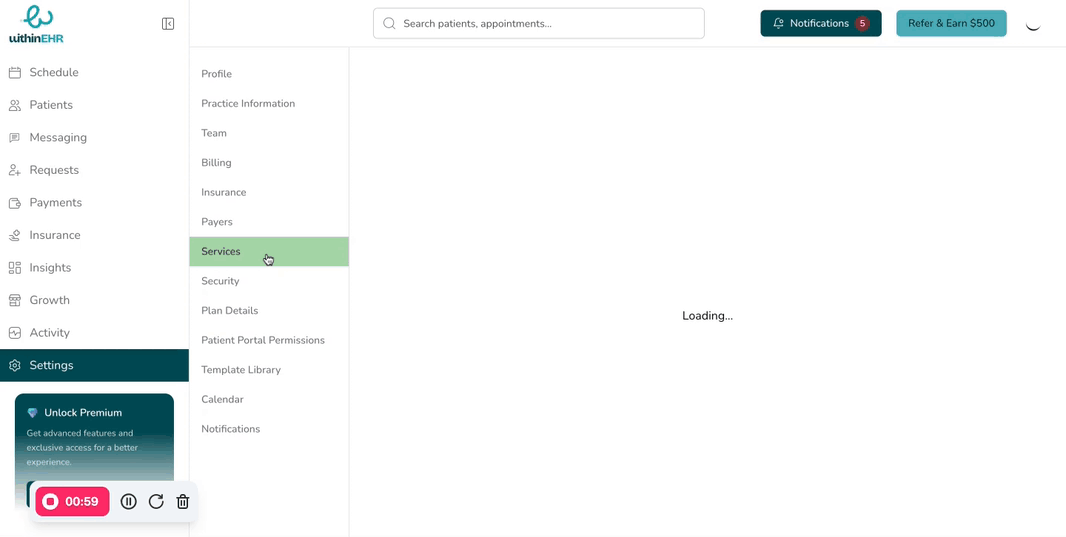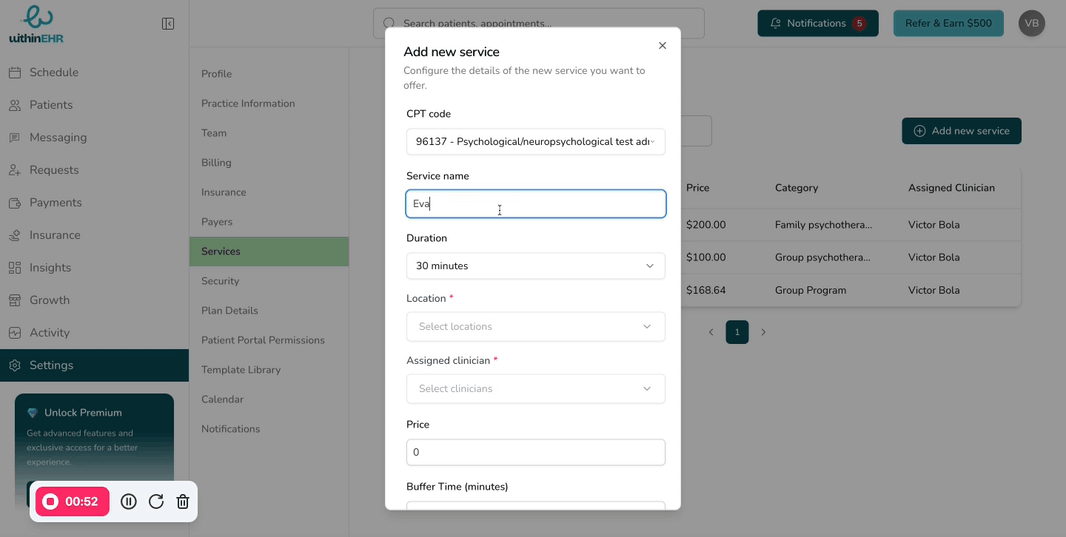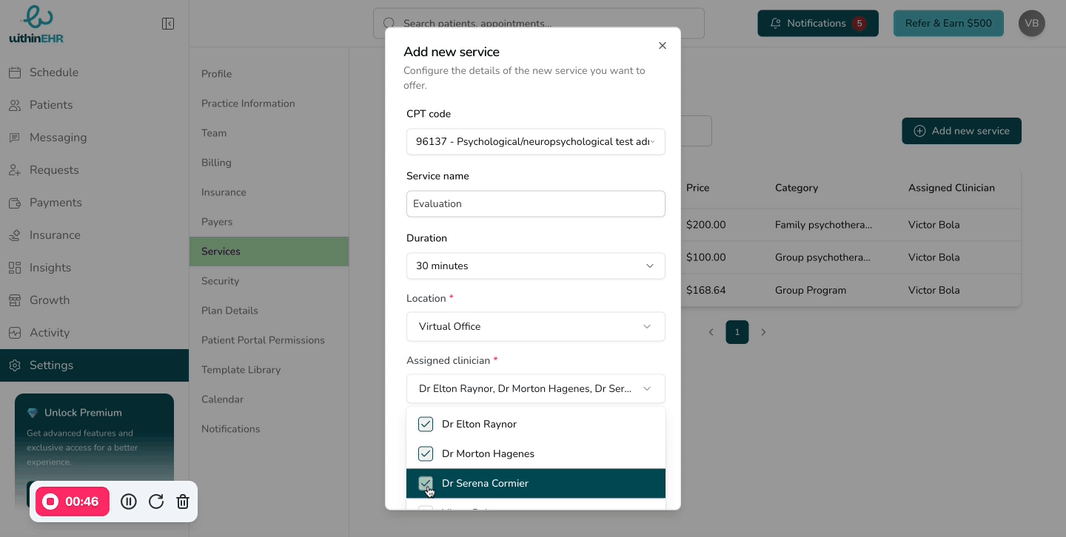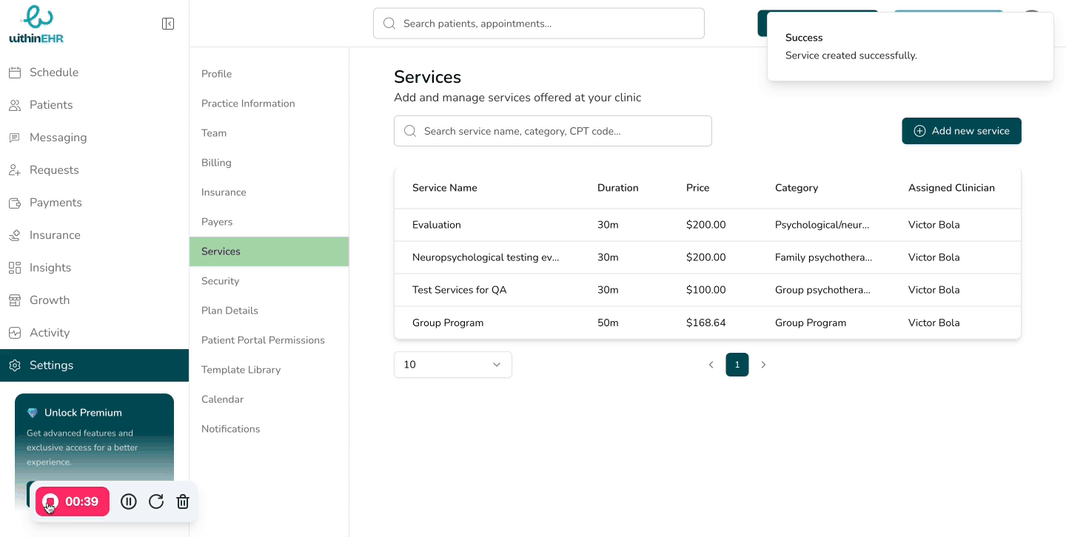
- Enter the team member's basic information.
- Click Continue to assign their role.
- Click Continue to add clinical information.
- Click Continue to review all details.
- Click Send Invitation to invite the new team member.
Team Roles in WithinEHR
Clinician
Clinicians are the healthcare professionals responsible for direct patient care. Their responsibilities include:
- Conducting assessments, diagnoses, and treatment planning
- Prescribing medications and performing clinical procedures
- Educating patients and coordinating with other providers
- Maintaining accurate, timely clinical documentation
Practice Manager
The Practice Manager oversees the business operations of the practice, including:
- Workflow optimization and facility management
- Financial management, budgeting, and revenue cycle oversight
- Staff hiring, scheduling, and performance management
- Regulatory compliance (HIPAA, PCI) and risk management
- Patient relations and strategic planning
Scheduler
The Scheduler manages appointment logistics and patient flow:
- Booking, rescheduling, and canceling appointments
- Verifying insurance and collecting patient information
- Managing provider calendars and preventing scheduling conflicts
- Coordinating referrals and communicating with patients about upcoming visits
Billing Specialist
The Billing Specialist ensures accurate and timely reimbursement:
- Translating clinical services into ICD-10 and CPT codes
- Submitting and tracking insurance claims
- Managing denials, appeals, and payment posting
- Communicating with patients about balances and payment plans
Supervisor
The Supervisor bridges clinical operations and staff management:
- Overseeing daily operations and quality assurance
- Managing staff schedules and performance evaluations
- Ensuring compliance with healthcare regulations and safety standards
- Acting as the communication link between frontline staff and management
Granting Permissions
- Click Settings on the navigation pane.
- Select Team.
- Choose the team member you want to update.
- Click Show Permissions at the bottom of the screen.
- Select the permissions you want to grant.
Assigning Services and Availability
Linking services and availability to each team member ensures clients can only book with providers who are qualified and available for that specific service.
- Click Settings on the navigation pane.
- Select Team.
- Choose the team member.
- Click Edit to add services.
- Click Save to update their services and availability.